What if the traditional “watchful waiting” approach to your child’s weight is actually more risky than taking proactive, medical action? As a parent, you want the best for your child, but the path toward helping my child lose weight safely often feels cluttered with conflicting advice and the fear of saying the wrong thing. You’re likely worried about the emotional toll of bullying or the looming threat of Type 2 diabetes, especially since 21.1% of U.S. children now face obesity. It’s natural to feel overwhelmed when balancing their physical health with their self-esteem.
We’re here to provide a clear, science-backed roadmap that prioritizes metabolic health and emotional well-being over simple calorie counting. You’ll discover how the latest 2026 AAP clinical guidelines recommend a more proactive stance, including specialized pediatric programs and FDA-approved interventions for those twelve and older. This article outlines exactly how to transition from anxiety to action, ensuring your family has the tools to support healthy growth while protecting your child’s confidence. We view this journey as a collaborative partnership between medical science and your family’s unique needs.
Key Takeaways
- Learn why BMI centiles are the gold standard for tracking pediatric health and how they differ from adult weight metrics.
- Understand the physiological importance of growth-preserving nutrition when helping my child lose weight safely to protect their long-term development.
- Discover age-appropriate strategies that balance your guidance with your child’s increasing need for autonomy and healthy self-esteem.
- Identify the metabolic “red flags” that indicate it’s time to transition from home-based changes to professional clinical intervention.
- Explore how a multi-disciplinary team of specialists can provide the customized medical oversight your child needs for sustainable results.
Understanding Pediatric Weight and Health Metrics in 2026
When you look at a growth chart, it’s easy to feel overwhelmed by the numbers. Traditional weight measurements don’t tell the whole story for a developing body. We now understand that Understanding Pediatric Weight and Health Metrics requires looking at growth-adjusted data rather than just a static number on a scale. Since approximately 21.1% of U.S. children are currently classified as obese, clinical precision is more important than ever. Helping my child lose weight safely starts with recognizing that their body is a moving target, constantly shifting in composition as they age.
The old “wait and see” approach is often a medical risk. We used to dismiss extra weight as “baby fat” that a child would eventually outgrow. However, modern clinical evidence suggests that early intervention is key to preventing metabolic shifts that become harder to reverse later. By focusing on health metrics like energy levels, sleep quality, and respiratory ease, we can build a comprehensive picture of your child’s physiological state. We prioritize these markers because they reflect the internal health of your child, not just their outward appearance.
To better understand the nuances of managing your child’s weight, watch this helpful video:
Calculating and Interpreting BMI Centiles
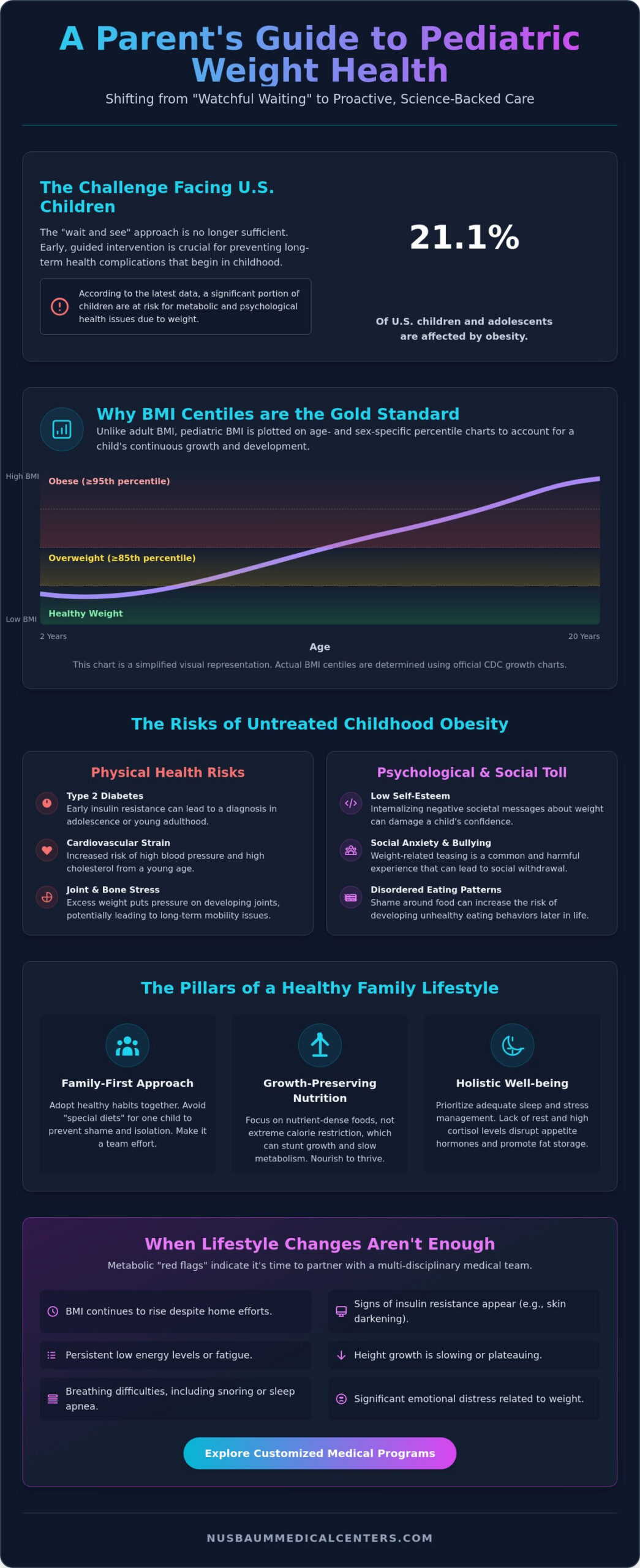
Adult BMI calculations are straightforward, but pediatric metrics must account for age and sex. This is why we use BMI centiles, or percentiles. If your child is in the 90th percentile, it means their BMI is higher than 90% of children of the same age and gender. These charts allow us to track how your child is growing relative to their peers, ensuring that weight loss doesn’t interfere with height velocity or bone density. The CDC defines a BMI at or above the 85th percentile but below the 95th as overweight, while a BMI at or above the 95th percentile is classified as obese.
The Long-Term Health Implications of Early Obesity
The risks of untreated childhood obesity extend far beyond physical appearance. We see a direct link between early weight struggles and the development of insulin resistance, which can lead to early-onset Type 2 diabetes. Developing bodies also face significant cardiovascular strain and joint stress that can impact mobility for decades. Beyond the physical, the psychological toll is profound. Social anxiety and low self-esteem often stem from weight-related bullying. By addressing these issues early through a structured pediatric weight loss program, we can protect both their metabolic health and their emotional resilience.
The Physiological Foundation of Safe Weight Loss for Children
Helping my child lose weight safely requires a shift in perspective. We aren’t just looking at a number on a scale; we’re protecting a biological blueprint that’s still being written. Extreme caloric restriction is dangerous for children because it can stunt linear growth and impair cognitive development. Instead, we focus on metabolic optimization. If a child’s body perceives a famine through severe restriction, it may slow down the metabolism to protect vital organs, making long-term progress nearly impossible. Our goal is to nourish the body so it feels safe enough to release excess weight.
Success rarely happens in isolation. We advocate for a “Family-First” approach where every household member adopts healthier patterns. When a child is singled out with a “special diet,” it creates a sense of shame and increases the risk of disordered eating later in life. By making collective changes, you normalize healthy habits and remove the psychological burden from your child. This supportive environment is the most effective way to ensure lasting change while protecting their emotional well-being.
Don’t overlook the impact of sleep and stress on your child’s physiology. Lack of rest disrupts the delicate balance of hormones that control appetite. High stress levels increase cortisol, which signals the body to store fat, particularly in the abdominal area. We find that stabilizing these lifestyle factors often provides the necessary foundation for medical interventions to work more effectively.
Macro-Nutrients for Developing Bodies
We prioritize high-quality protein and healthy fats to support bone density and brain health. Many school lunches contain “hidden sugars” that spike insulin and lead to energy crashes, which often trigger overeating later in the day. We recommend replacing juice and sports drinks with water or electrolyte-rich infusions to maintain hydration without the glycemic load. If you feel your family needs more structured support, our pediatric weight loss program provides the clinical framework to make these nutritional shifts sustainable.
The Role of Hormones in Childhood Weight
Hunger isn’t just about willpower; it’s a hormonal signal. Leptin tells the brain when the body has enough energy stored, while ghrelin signals hunger. In children with obesity, these signals often become cross-wired, leading to persistent hunger even after a meal. We also monitor for conditions like Polycystic Ovary Syndrome (PCOS) in adolescent girls, which can make weight management significantly more difficult without specialized care. Professional medical oversight ensures we’re treating the underlying physiology rather than just the outward symptoms.
Age-Specific Strategies for Helping Your Child
Effective strategies for helping my child lose weight safely depend heavily on their current stage of development. What works for a seven-year-old will likely backfire with a seventeen-year-old. We emphasize a shift from total parental control toward a collaborative partnership as your child matures. Creating “Safe Zones” in your home is a vital first step; this means ensuring that the easiest choice is always the healthiest one. By stocking the pantry with whole foods and removing the allure of certain snacks, you reduce the daily friction of decision-making for your child.
The language we use at home shapes a child’s internal monologue for years to come. We recommend focusing entirely on “fueling for performance” and “building strength” rather than discussing the scale or clothing sizes. When you remove words like “fat” or “diet” from the household vocabulary, you help your child associate health with vitality rather than restriction. This approach protects their emotional well-being while they make necessary physiological adjustments. We view you as the primary architect of their environment.
Strategies for School-Age Children (Ages 7-10)
For this age group, movement should never feel like a chore. We prioritize play-based exercise, such as family bike rides, swimming, or active games like tag, which build cardiovascular health without the pressure of a structured gym environment. Engaging children in meal preparation and grocery shopping gives them a sense of ownership over their choices. They’re more likely to eat a vegetable they helped select. When celebrating achievements, we suggest using non-food rewards. A trip to the park or a new book provides positive reinforcement without reinforcing the emotional connection between food and reward.
Supporting the Adolescent and Teen Years (Ages 11-17)
Adolescence brings a new set of challenges, particularly the influence of social media on body image. We encourage open dialogue about how digital filters often present unrealistic standards. Your teen needs autonomy. As they gain more independence, they face eating decisions at school and with friends. We guide them to make empowered choices by focusing on how different foods affect their energy levels and focus. If lifestyle changes aren’t producing the desired metabolic shifts, it may be time to introduce more structured medical weight loss nj concepts. This transition allows for professional oversight while respecting your teen’s growing need for independence in their health journey.
When Lifestyle Changes Aren’t Enough: Medical Intervention
Sometimes, even the most dedicated family efforts don’t yield the expected results. If you’ve been focused on helping my child lose weight safely through nutritional shifts and active play but see no change in their BMI centile, it’s time to look deeper into the underlying biology. Pediatric obesity is a complex, chronic disease. It isn’t a failure of willpower or parenting. We see many cases where a child’s metabolic set point is biologically resistant to standard lifestyle changes. In these instances, professional medical intervention isn’t just an option; it’s a necessary step to protect their long-term health.
The evolution of pediatric weight management has moved far beyond the simplistic “eat less, move more” mantra. We now understand that genetics and hormonal signaling play a massive role in how a child’s body stores and uses energy. When lifestyle modifications aren’t enough to move the needle, we utilize clinical tools that address the physiological drivers of weight gain. This proactive approach helps prevent the development of comorbidities like Type 2 diabetes or hypertension before they become permanent fixtures in your child’s life.
Identifying Clinical Resistance
Clinical resistance occurs when a child’s body actively fights weight loss through metabolic adaptation. This can happen due to genetic predispositions or the hormonal imbalances we discussed in previous sections. Red flags include persistent high blood pressure, signs of insulin resistance like skin darkening around the neck, or sleep apnea. When a child’s BMI remains at or above the 95th percentile despite consistent lifestyle modifications, a pediatrician should refer the family to a specialized weight loss program. These specialists can run advanced metabolic panels to identify exactly where the biological blockages are occurring.
The Role of Medically Supervised Programs
Specialized programs differ significantly from adult weight loss clinics because they prioritize growth preservation. We ensure that any intervention supports height velocity and bone development. According to the updated 2026 American Academy of Pediatrics guidelines, a more proactive stance is recommended for children facing severe obesity. For adolescents twelve and older, this may include FDA-approved medications like injectable semaglutide or liraglutide. These treatments work by mimicking natural hormones to regulate appetite and improve insulin sensitivity, creating a more favorable metabolic environment.
Medical intervention is a comprehensive strategy that integrates nutritional counseling and behavioral therapy with clinical oversight. We monitor every marker to ensure the process of helping my child lose weight safely is both effective and growth-appropriate. If you’re ready for an expert partner in your child’s health, we invite you to learn more about our Pediatric Weight Loss Program. This multidisciplinary oversight provides the safety net your child needs for sustainable, long-term success.
Partnering with a Pediatric Weight Loss Specialist in NJ
Choosing to work with a specialist is a significant step toward helping my child lose weight safely. When you enter a clinical setting dedicated to pediatric health, the experience differs fundamentally from a standard checkup. Your first visit focuses on a comprehensive metabolic assessment rather than just a number on a scale. We analyze blood work, growth history, and lifestyle patterns to understand the “why” behind your child’s weight. This deep dive allows us to move past generic advice and create a precise medical plan tailored to your child’s unique physiology.
A successful outcome requires more than just a doctor’s visit. It takes a multi-disciplinary team. Our approach integrates the expertise of medical doctors, registered dietitians, and health coaches who work in tandem to support your family. While the physician oversees clinical interventions and metabolic health, dietitians provide actionable nutritional roadmaps and coaches offer the behavioral support needed to maintain momentum. This collective oversight ensures that every aspect of your child’s development is monitored and protected.
Initiating the conversation with your child requires a delicate balance of clinical honesty and parental warmth. We suggest framing the specialist as a “health coach” or a “growth partner” who helps the body work at its best. Focus the discussion on how the program will help them feel more energetic and stronger for the activities they love. By positioning the medical team as a resource for vitality, you remove the stigma and invite your child to be an active participant in their own wellness journey.
The Nusbaum Approach to Pediatric Health
At our centers in Morristown and Cedar Knolls, we provide a high-end, supportive environment where clinical excellence meets deep empathy. We understand the local challenges North Jersey families face, from busy school schedules to the pressures of social environments. Our pediatric weight loss program balances advanced medical interventions with positive psychological support. We’ve seen real results for families who previously felt stuck, helping children regain their confidence while optimizing their metabolic markers.
Creating a Sustainable Family Roadmap
We don’t believe in quick fixes that fail after a few months. Your journey begins with a clear roadmap for the first 90 days, focusing on stabilizing insulin levels and establishing consistent movement patterns. We set realistic, health-based goals that celebrate progress in energy, sleep quality, and physical capability. Long-term success is built on regular follow-ups that allow us to adjust the plan as your child grows and their needs evolve. If you’re ready to move toward a healthier future, book a consultation today to start your child’s journey toward medical weight loss nj.
Empowering Your Child’s Healthy Future
Taking the first step toward clinical intervention is a profound act of care. We understand that the path toward helping my child lose weight safely is often filled with uncertainty, but you don’t have to navigate it alone. By shifting the focus from simple caloric restriction to metabolic optimization and growth preservation, you provide your child with the foundation they need for a vibrant life. Whether it’s through age-appropriate lifestyle shifts or medically supervised treatments for adolescents, the goal is always sustainable health and restored confidence.
Led by Dr. Michael Nusbaum, a Board-Certified Surgeon, our practice offers personalized, medically supervised pediatric programs designed to meet your family’s specific needs. With convenient locations in Morristown and Cedar Knolls, we act as both rigorous scientists and dedicated coaches in your child’s health journey. We invite you to Schedule a Pediatric Weight Loss Consultation in NJ today. A healthier, more energetic future for your child is possible through expert guidance and specialized care.
Frequently Asked Questions
Is it safe for a child to go on a weight loss diet?
Restrictive dieting is generally unsafe for children because it can interfere with linear growth and cognitive development. Instead of traditional dieting, we focus on nutritional optimization that supports metabolic health while ensuring your child receives adequate macro-nutrients for bone and brain development. Helping my child lose weight safely involves shifting away from calorie counting toward a family-wide focus on whole foods and metabolic stability.
How can I tell if my child is “obese” or just has “baby fat”?
You can distinguish between temporary growth patterns and clinical obesity by using age-specific and sex-specific BMI centiles. While “baby fat” is common in early childhood, a BMI at or above the 95th percentile indicates a clinical need for intervention according to 2026 AAP guidelines. Our team uses these growth-adjusted metrics to determine if your child’s weight poses a long-term risk to their cardiovascular and metabolic health.
Can my teenager use weight loss medications like Semaglutide?
Yes, teenagers aged 12 and older may be candidates for FDA-approved medications like semaglutide if they meet specific clinical criteria. These medications are indicated for adolescents with a BMI at or above the 95th percentile and are most effective when integrated into a comprehensive pediatric weight loss program. We provide the clinical oversight necessary to monitor your teen’s progress and ensure the medication supports their overall physiological development.
What is the best exercise for a child who is overweight?
The best exercise for an overweight child is play-based movement that they genuinely enjoy rather than structured, high-intensity workouts. Activities like swimming, family bike rides, or active games reduce the physical strain on developing joints while improving cardiovascular health and insulin sensitivity. We encourage daily physical activity that feels like fun, which helps build a positive relationship with movement and supports long-term weight maintenance.
How do I talk to my child about their weight without hurting their feelings?
You should focus the conversation on health, strength, and energy levels rather than using words like “weight” or “fat.” Explain that the goal is to help their body work at its best so they have more energy for the things they love to do. This approach validates their feelings while framing medical support as a positive tool for vitality and long-term well-being rather than a punishment for their appearance.
What happens during a pediatric weight loss consultation?
During a consultation, we perform a thorough metabolic assessment that includes a review of your child’s growth history and current health markers. We discuss your family’s lifestyle patterns and identify any biological or environmental barriers to success that may be hindering progress. This information allows us to create a personalized roadmap that may include nutritional guidance, behavioral support, or medical interventions tailored specifically to your child’s unique needs.
Are pediatric weight loss programs covered by insurance in NJ?
Insurance coverage for pediatric weight management varies by provider, but New Jersey legislation introduced in February 2026, Bill S3549, aims to mandate coverage for obesity treatments. This includes preventive care, counseling, and anti-obesity medications for eligible patients. We recommend contacting your insurance carrier to understand your specific benefits, as many plans are expanding their support for comprehensive metabolic care to address the 21.1% childhood obesity rate.
How long does it typically take to see results in a pediatric program?
Most families begin to see positive shifts in energy levels and metabolic markers within the first 90 days of a structured program. Helping my child lose weight safely is a steady process that prioritizes long-term health over rapid, unsustainable changes. We focus on consistent progress in health metrics and lifestyle habits, ensuring your child reaches a healthy weight while continuing to grow and thrive throughout their developmental years.

